Emergence
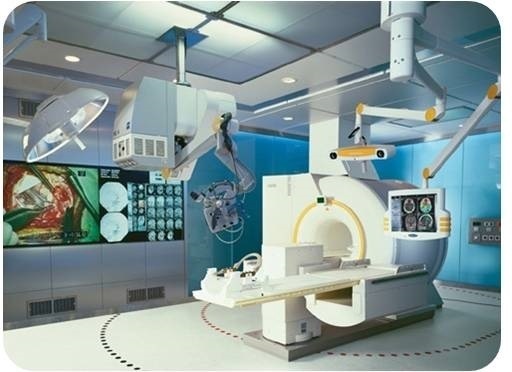
Somewhere in the depths of my sleep I heard a noise. The noise was persistent. Slowly I emerged from a deep slumber and identified the noise as my ringing mobile phone. Then further time lapsed until I arrived at sufficient awareness to acknowledge that I was in fact a neurosurgeon and I was on emergency call. I groaned and my wife murmured and turned over to face the opposite side – a routine that had played itself out repeatedly through all the times that I had been on emergency call over twenty five years of marriage (now thirty five years!). I squinted at the clock. Four twenty am, for shit’s sake! I took the call.
“Is that Dr Weinberg?” enquired the voice.
“Yes. Who wants to know?” I grunted.
“This is the ER at the Meddowdale Hospital. We’ve just admitted an MVA (motor vehicle accident) case – a woman in her late forties. Clinically unresponsive with fixed pupils (non-reactive to light) and currently being ventilated. A CT scan performed on admission reveals a traumatic subarachnoid hemorhage. Essentially brain-dead.” she rattled off.
I was now adequately awake to be able to comprehend the clinical picture. I responded. “ So you’ve woken me up at 4.20am just to inform me that you have a brain-dead MVA case, knowing that since it’s a traumatic subarachnoid, there’s no indication for neurosurgical intervention”, I barked (and the wife groaned).
“Apologies doctor. Agreed. Just thought to inform you since you’re the consultant on call. We’ll do the necessary.” She responded.
“Thanks awfully” I answered. Dropped the phone on the bedside table, turned over and attempted to go back to sleep.
But sleep wouldn’t come. In its place an inexplicable disquiet began to emerge from some deep, subliminal space. There was something wrong. Something very wrong with this case. There was nothing in the details. Just an undercurrent of something that just didn’t sit well. After agonizing for a half an hour I decided that I had to go and assess the brain-dead patient for myself. I got dressed, braved the freezing winter morning and headed out to the hospital.
I arrived at the ER and sought the doctor that had called me. I was directed to a cubicle where I found the said colleague talking to a distraught man. She was advising him to notify his church and funeral company about the imminent death of his wife and to make the necessary arrangements. On seeing me appear, as if an apparition emerging from the mist, the wide-eyed colleague (actually beautiful-eyed as I recall) introduced me to the husband. I requested to see the patient before I expressed any opinion and was referred on to the Intensive Care Unit. And there for the first time I met Lorna. She was indeed in a bad way – deeply comatose. But ...... as I worked my way through the clinical assessment, I morphed into ‘surgical mode’ with welling anger. The case had been wrongly assessed. I was now furious and in full neurosurgical ‘fight mode’. The patient was indeed responsive to pain. There was a flicker of a response to light in the right pupil. Off the ventilator she took some spontaneous breaths. But most of all, the CT scan revealed a large, actively bleeding subdural hemorhage and not subarachnoid hemorhage. In other words, the blood was layered over the surface of the brain and not within the fluid areas inside the brain. The large collection was severely compressing the brain. The difference between the two types of hemorhages was that the subdural collection was potentially curable. The surgery for this bleed is invariably LIFE SAVING!
What a balls-up! I was now raging. While yelling at the gorgeous-eyed ER doctor (whose eyes were now a little redder and moister) and accusing her of mismanaging the case, I managed to explain to husband Hank, that there was a chance that I could save his wife with emergency surgery. Then called my faithful anaesthesiologist and got the OR prepared for a craniotomy (skull-opening procedure).
Patient on the table. Head clamped. Shaved, cleaned, draped. And before you knew it, I was in the head. There was a linear fracture along the length of the bone window that I sawed out. The dura mater (the membrane covering the brain) was bulging with the pressure of the underlying hemorhage. I incised the dura and released the pressurized clot, followed by active hemorhage. The brain was severely compressed and had a nasty red color. I began the pain-staking search for the source of the hemorhage. The path of active bleeding led me to a cortical vein (vein running along the surface of the brain) which had torn off from a major draining sinus (a large venous draining vessel enclosed within the dura mater). I managed to cauterize the stump of the torn vessel leading into the sinus as well as the cortical vessel itself.
At this time the brain began to swell. This was most likely a combination of the trauma itself which had caused brain contusion (bruising) as well as a reaction to the severe compression of the pre-existing hemorhage. With urgency therefore I started closing the head. I left a pressure monitoring transducer in the space between the brain and the dura (intra-cranial pressure monitoring) so that we could monitor and treat the pressure over the next several days. The patient would be maintained in a deeply sedated state with full mechanical ventilation and other life support functions. Of primary importance was the management of intra-cranial pressure. On completing the procedure, the patient was moved to the Intensive Care Unit.
For the first time now I had the opportunity to chat with husband Hank. I indicated that we were in with a chance of saving Lorna. However, much depended on the ability to reverse the brain swelling and associated pressure. Even if Lorna’s life was saved, I feared there would be significant neurological deficits, with degrees of irreversibility. There was a long road ahead.
I asked Hank about Lorna. He indicated that she was a highly successful businesswoman, on the executive of a large corporate. And then he shared the gut-wrenching information. He had recently found out that Lorna was having an affair with a much younger guy at work. Lorna and her young partner had been partying the previous evening and it was in fact the inebriated partner that had been behind the wheel when the car rolled on the freeway. He was apparently unhurt and nowhere to be found. Hank began to weep. He was broken. It was just too much!
“I’m so sorry Hank,” I said, putting my hand on his shoulder. Hell, I really felt this man’s pain.
“I really love her. I’m with her all the way. Whatever it takes.” he said.
“It’s a long road ahead, Hank. But we’ll support the process with all our resources. I also think that you should consider consulting an appropriate professional for some counselling.” I responded. Hank nodded.
Lorna regained consciousness one week later. She had a severe weakness over half her body together with an expressive speech deficit. The acute care was followed by intensive rehabilitation. Lorna made good progress in the face of what had been a life-threatening injury. However she remained with a spastic-type hemiparesis (weakness of arm and leg) and slurred speech. She was never able to return to work again. As for the young beau who was really responsible for all of this, he had disappeared into thin air.
Hank is the true hero of this tale. He stuck by Lorna throughout the acute care, the months of rehabilitation and beyond. Every so often I’m consulted by Lorna regarding various problems which have arisen. And always by her side is Hank. His fortitude and unconditional loyalty is truly the great inspiration of this human drama.
"Articles from Ian Weinberg
View blog
If I were to ask you how you view yourself you would probably respond with a description which is a ...

From time to time I manage to get off the train of life for short periods of reflection. It became a ...
So there was this virus that originated in Wuhan and spread around the globe. The virus differed fro ...
Related professionals
You may be interested in these jobs
-

Payroll Administrator
Found in: Job Placements ZA C2 - 5 days ago
People Dimension Boksburg, South Africa Full timeJob Description/Duties: · Working out driver salaries. · Paying salaries on the inhouse system. · Working with South Africa and Zimbabwe's deductions. · Minimum Requirements: · Dedicated. · Being dynamic. · Being detail orientated. · Have a good work ethic. · Be proficient in Mic ...
-
Data Analyst
Found in: Talent ZA 2A C2 - 23 hours ago
Network Recruitment Johannesburg, South AfricaAs a Data Analyst you will be responsible for analyzing large sets of financial data to support our business operations and drive data-driven decision making. · Responsibilities:Collect, organize and analyze large sets of data related to the bank's financial operations · Develop ...
-
Product Specialist
Found in: Talent ZA C2 - 5 days ago
StaffAtAClick (Pty) Ltd Johannesburg, South Africa Full timeDuties and Responsibilities · Client interaction (internal and external clients) · Trouble shooting and user support · Software testing · New client setup /configuration on the SDM system · Data processing, analysis and manipulation in Excel · Qualifications and Experience · Mini ...


 Ltd&v=024)
Comments
Cyndi wilkins
6 years ago #25
Ian Weinberg
6 years ago #24
Cyndi wilkins As you may have gleaned from my collective writings I am very much a proponent of other elements, including neurophysics which give rise to the human state. However we need to respect a hierarchical structure starting with anatomy and physiology at the foundation. Upon that we can build the mind- body influences (PNI) which I pioneered in the clinical domain. Then we can add in the energy interface with nonlocality. At the latter level exists resonance and not cause and effect. But to take the resonant energetic connections from nonlocality and imbibe functional significance to physical elements is incorrect. In other words energetic grids may incorporate the heart in nonlocality integrations but in physicality the heart is a muscular pump which generates a strong electric field (ECG) - it 'expresses' and amplifies mind cognition and emotion and in turn, influences the mind-brain electrically and via autonomic connections. But at the pure physical level the heart as an organ has no intrinsic emotional or cognitive function.
Ian Weinberg
6 years ago #23
As you may have gleaned from my collective writings Cyndi wilkins I am very much a proponent of other elements, including neurophysics which give rise to the human state. However we need to respect a hierarchical structure starting with anatomy and physiology at the foundation. Upon that we can build the mind- body influences (PNI-which I pioneered in the clinical domain. Then we can add in the energy interface with nonlocality. At the latter level exists resonance and not cause and effect. But to take the resonant energetic connections from nonlocality and imbibe functional significance to physical elements is incorrect. In other words energetic grids may incorporate the heart in nonlocality integrations but in physicality the heart is a muscular pump which generates a strong electric field (ECG) - it 'expresses' and amplifies mind cognition and emotion and in turn, influences the mind-brain electrically and via autonomic connections.
Cyndi wilkins
6 years ago #22
Ian Weinberg
6 years ago #21
Cyndi wilkins The heart is not a cognitive/emotional brain. It is a muscular pump with an intrinsic electro-chemical circuit controlling heart rate and rhythm. It secretes a diuretic hormone. It also generates a powerful electric field within the body (as a volume conductor). It would then influence the brain because the brain exists within the range of the electric field. The sequence then is that the cognitive and emotional brain influences the heart neurologically (autonomic nervous system) and chemically via hormones and immune system secretion. The heart electric field reflecting rate, rhythm and amplitude then influences neuronal networks within the brain, in turn affecting cognition and emotion. I have done much research on the influences of mind states on the body electric field (see http://www.pninet.com/articles/Electro-couple.pdf ). This may be a bit technical - a proposed model. There is also no brain in the gut/abdomen. There is a neural network in the bowel wall which interacts with the autonomic nervous system - efferently (transmission from brain to gut) as well as afferently (gut to brain). The gut is also influences by hormones and immune chemistry.
Ian Weinberg
6 years ago #20
Cyndi wilkins The heart is not a cognitive/emotional brain. It is a muscular pump with an intrinsic electro-chemical circuit controlling heart rhythm. It secretes a diuretic hormone. It also generates a powerful electric field within the body (as a volume conductor). It would then influence the brain because the brain exists within the range of the electric field. The sequence then is that the cognitive and emotional brain influences the heart neurologically (autonomic nervous system) and chemically via hormones and immune system secretion. I have done much research on the influences of mind states on the body electric field (see http://www.pninet.com/articles/Electro-couple.pdf ). This may be a bit technical - a proposed model. There is also no brain in the gut/abdomen. There is a neural network in the bowel wall which interacts with the autonomic nervous system - efferently (transmission from brain to gut) as well as afferently (gut to brain). The gut is also influences by hormaones and immune chemistry.
Ian Weinberg
6 years ago #19
Cyndi wilkins
6 years ago #18
Cyndi wilkins
6 years ago #17
Not sure how one might go about lobotomizing one's intuitive energies, which metaphorically speaking is in reference to the 'gut brain' or trusting one's instincts and such...but I suppose where there is a will there is a way...Electric shock therapy might do the trick;-) #19 All kidding aside...If you have not tried it already...A bit of warm water and lemon first thing in the morning may help to tame your 'naughty bowels' Ken Boddie;-)
Ken Boddie
6 years ago #16
Far be it from me, Ian, to query your self diagnosis, but when my "bowels knot up" it's the space at my non thinking end that takes flight ..... and fast. 🤢
Ian Weinberg
6 years ago #15
some have claimed that we have a gut brain. But in my years spent navigating the abdomen as a general surgeon, I never found anything to lobotomize. In my case, when my bowels knot up, I feel that unique queeziness which somehow tickles my fight/flight centre in the space between my ears!
Ken Boddie
6 years ago #14
Cyndi wilkins
6 years ago #13
With all due respect to Hank for sticking by his badly injured wife...and to you Dr. Weinberg for having saved her life...Had that ER doctor not checked her work by making 'the call'...that young woman would be dead right now. Perhaps the real hero of this story is in trusting one's intuition;-)
Ian Weinberg
6 years ago #12
Thanks for those kind words Jerry Fletcher
Jerry Fletcher
6 years ago #11
Ian Weinberg
6 years ago #10
Thanks Aaron \ud83d\udc1d Skogen Fortunately I'm sensitive to an active gut feel - got me out of many a tight situation.
Ian Weinberg
6 years ago #9
Thanks Cyndi wilkins Indeed you are perfectly correct. I was judgemental in the heat of the moment. But there is always the bigger (higher) perspective.
Cyndi wilkins
6 years ago #8
Ian Weinberg
6 years ago #7
Thanks Chas \u270c\ufe0f Wyatt
Ian Weinberg
6 years ago #6
Thanks again Pascal Derrien
Pascal Derrien
6 years ago #5
Ian Weinberg
6 years ago #4
Thanks so much for the kind words Humbled. Thanks also for sharing.
David B. Grinberg
6 years ago #3
Ian Weinberg
6 years ago #2
No. Just a sign that says 'Room Service'. Called 20 mins ago by the ward sister (woken at 4.27am) - patient demanding something urgently for constipation!!!
Paul Walters
6 years ago #1